|
Disposable scopes differ from traditional flexible bronchoscopes in that they have an integrated video processing unit/light source and do not require an external source. In recent years, single use disposable flexible bronchoscopes have been introduced. Syringes with lidocaine should include air at the top to ensure the contents of the syringe are flushed completely through the working channel. The lidocaine administration is usually via 10 cc slip tip syringes. In addition, adequate syringes for lidocaine administration will be necessary. 
Alternatively, a Luer lock syringe can be modified by simply cutting off the threaded portion which results in a slip tip syringe. If a slip tip syringe is not available, a Luer lock syringe can be used with an adaptor. These are usually 20 or 60 cc slip tip syringes that insert into the biopsy port on a bronchoscope. If a larger diameter therapeutic flexible bronchoscope is required for a procedure (e.g., removal of blood clots), and the patient has a smaller than adequate ET tube, then upsizing the ET tube will be necessary.įor diagnostic procedures, the most frequent equipment needed is setup for a bronchoalveolar lavage. This prevents high airway pressures, ensures adequate ventilation, and avoids scope damage ( 2, 3). of the bronchoscope and inner diameter (I.D.) of the ET tube is recommended. When inserted into an ET tube, a clearance of >2 mm between the O.D. 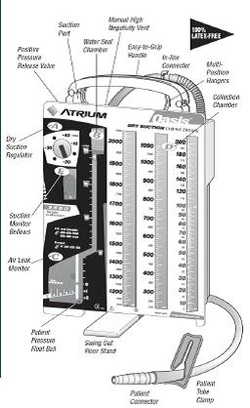
LMA, laryngeal mask airway.įlexible bronchoscopes range in O.D. Note the bite block present around the LMA to prevent scope damage. At the beginning of every procedure, a bite block should be placed to prevent damage to the bronchoscope irrespective of the patient’s level of sedation or use of neuromuscular blockade.Īn example of a bronchoscope set up with a ventilator connected to an LMA via a swivel adaptor. The patient’s vital signs monitor is also adjusted in line with the proceduralist’s visual field to allow real time patient vital signs monitoring. In order to create space for the bronchoscopist at the head end of the bed, the patient’s bed, ventilator and intravenous line setups need to be moved. With the image inversion, the bronchoscopist adjusts for anatomy when performing any therapeutic interventions. With the operator at the side of the bed, the patient’s left mainstem is seen on the right side of the monitor and the posterior tracheal wall is now on the upper part of the screen ( Figure 1). This contrasts with the bronchoscopic image when the operator stands at the side of the bed and the bronchoscopic image on the monitor is inverted. When the operator is at the head end of the bed, the bronchoscopic image visualized on the monitor shows the left mainstem on the left side of the monitor, and the anterior tracheal wall is on the upper part of the screen. FB is typically done at the head of the bed, though it is often also done from the side of the bed especially in intubated patients in ICU. Anecdotally, patients’ fraction of inspired oxygen (FiO 2) is increased to 100% for the duration of the procedure. The patient is placed in a supine position with the ventilator in a controlled mode. The bronchoscopy tower or disposable bronchoscope screen should be setup at the patient’s bedside in the ICU. The first and most important step is to ensure that all needed equipment and supplies are readily available. We further briefly describe the additional equipment needed for specialized techniques in therapeutic bronchoscopy used by interventional pulmonologists.įB is frequently performed in an ICU setting. The components of procedural setup are discussed in relation to patient factors that include patient positioning and anesthesia, personnel in the procedure team and the equipment itself. 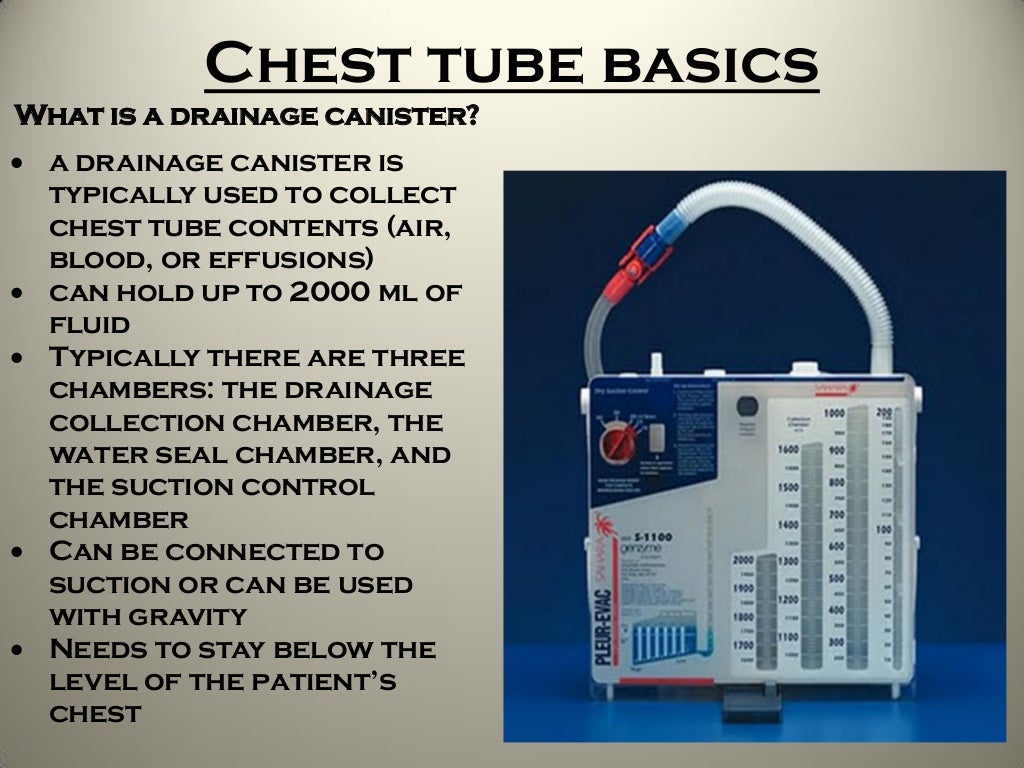
We provide a guide checklist for these procedures emphasizing the practical aspects of each procedure from selecting the appropriate size endotracheal tube to operator positioning to ensure efficiency and best access. These include flexible diagnostic and therapeutic bronchoscopy, ultrasound guided thoracentesis, chest tube insertion, difficult airway management, and bedside percutaneous dilatation tracheostomy. In this review we describe the equipment and procedural setup ideal for both pleural and airway procedures. 
This is especially essential to ensure patient safety, minimize risk of complications, and improve success for specialized procedures performed by interventional pulmonary in the intensive care unit. Taking the time to plan the procedure setup in advance and having all necessary equipment readily available at the patient’s bedside is imperative for procedural services. Interventional pulmonologists provide a procedural practice and have additional expertise in performing high-risk procedures needed in the critically ill patients in intensive care. Procedural setup is an important aspect of any procedure.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
